Sports-Related Injuries
Experience matters! Dr. Luga Podesta has the experience, knowledge and expertise necessary to get you back in the game at the highest level of competition. Sports related injuries can occur whether you are a competitive athlete, dancer, musician or a weekend warrior or homemaker. How those injuries are treated and heal will determine when, and to what extent, you can return to sports. Choosing the correct doctor to evaluate and treat your injuries is paramount returning you back to the field as quickly and safely as possible.

Common Sports Injuries
Shoulder Pain
- Bursitis
- Impingement
- Labral / SLAP Tears
- Rotator Cuff Tendinitis / Tears
- Biceps Tendonitis
- Dislocation / Instability / AC Joint Separation
Elbow Pain
- Common Flexor Tendonitis (Golfers Elbow)
- Common Extensor Tendonitis (Tennis Elbow)
- Ulnar Collateral Ligament Injury (UCL)
- Distal biceps tendonitis / tears
- Bursitis
- Nerve Injuries (Cubital Tunnel)
Hand/Wrist Pain
- Carpal Tunnel Syndrome
- De Quervain’s Tendonitis
- Triangular fibrocartilage complex (TFCC) tears
- Thumb Sprains
- Thumb CMC (Basal) Joint arthritis
- Trigger finger
Hip Pain
- Arthritis
- Labral tears
- Femoral acetabular impingement (FAI)
- Gluteal tendonitis
Knee Pain
- Patella / quadriceps tendonitis
- Hamstring tears
- Meniscus tears
- ACL / MCL tears
- Calf muscle strains
Ankle/Foot Pain
- Ankle sprains
- Achilles tendonitis /tears
- Posterior tibialis /Peroneal tendonitis
- Hallux rigidus / bunions
- Plantar fasciitis
Tendon Injuries
Tendon injuries can occur due to an acute injury that results in a partial of complete disruption of the tendon itself or its attachment on a bone or due to overuse and repetitive stress or trauma. A tendon is a cord like fibrous tissue structure that originates on a muscle and functions to attach a muscle to a bone providing movement and stability of a joint. Tendinitis is an acute inflammatory condition affecting tendons typically where they attach on a bone. Tendon injuries have been described by several names including tennis elbow, golfers’ elbow, jumpers’ knee or swimmers’ shoulder. Regardless of the name, tendinitis can be painful, debilitating and effect any tendon. Early treatment is extremely important to minimize the long-term risks and effects of tendon injury. Dr. Podesta is a regenerative orthopedic and sports medicine expert that can accurately diagnose these injuries and initiate a personalized treatment recommendation to stimulate and enhance tendon healing.
The most common parts of the body affected by tendinitis include:
Shoulder: Biceps, rotator cuff tendons
Elbow: Common flexor tendon (Golfers elbow); Common extensor tendon
(Tennis elbow)Hip: Gluteal tendons (Medius and Minimous Tendons)
Knee: Patella tendon, Quadriceps tendon, Hamstring and gastrocnemius
tendons.Ankle: Achilles, posterior tibialis tendons, peroneal tendons
Foot: Achilles tendon, plantar fascia
How are tendons treated?
The initial inflammatory phases of tendinitis are typically short lived and responsive to conservative treatment including rest, oral NSAID medications, therapeutic modalities such as ice and heat, physical therapy, and activity modification. However, when longer lasting, chronic or after tendinosis develops, more aggressive injection therapies or regenerative orthopedic procedures are required such as:
- Corticosteroid Injection: Cortisone injections have been used to relieve pain and treat inflammatory conditions like tendonitis for years. These injections are most often performed in the physician’s office. Cortisone is typically combined with local anesthetic medication such as lidocaine. Due to potential side effects and systemic risks such as muscle, tendon and ligament weakening, articular cartilage damage, bone death (avascular necrosis), nerve damage, infection and elevation of blood sugar in diabetics; the number of injections you can receive in a year are limited.
- Platelet Rich Plasma (PRP) Treatments: Platelet rich plasma therapy has become the treatment of choice for early tendonitis. PRP, is performed to stimulate and further enhance our natural healing response when injected in an injury by concentrating growth factor containing platelets and circulating progenitor cells in plasma ultimately reducing pain and increasing tendon function by decreasing inflammation, stimulating tendon healing and functional improvement.
- Bone Marrow Concentrate (BMC) or Lipoaspirate Treatment: The addition of BMC or lipoaspirate, and the stem cells or progenitor cells it provides, is commonly used in combination with PRP to enhance the anti-inflammatory and healing potential. Previously referred to as “Stem Cell Therapy”, progenitor cell-based treatments are reserved for more severe tendon conditions such as tendinosis, calcific tendinosis or partial tendon tears. Bone marrow concentrate and lipoaspirate in addition to PRP has shown promise to further diminish inflammation, promote and stimulate normal tendon growth not observed with PRP alone. Progenitor cell-based therapy is performed in regenerative orthopedics to enhance the body’s natural healing mechanisms and capabilities to treat orthopedic conditions involving tendons throughout the body.
- Autologous Conditioned Serum: Autologous conditioned serum is performed by drawing a small sample of a patient’s own blood, allowed to remain in a clotted for at body temperature for 4 hours, centrifuged to separate the clot from its serum. The serum, which contains increased levels of autologous interleukin one receptor antagonist is the injected back into the injured joint or tissue within 6 hours of the initial blood draw. IL1RA has been used in Europe since 2003 under the names Orthokine and Regenokine, is currently under investigation for the treatment of inflammatory conditions involving tendons, ligaments and joints as a more physiologically natural and safer alternative to corticosteroids.
- Amniotic Fluid Allographs: Amniotic tissue and amniotic membrane is a protective barrier in the human placenta. It is typically discarded after a baby is delivered. There is scientific evidence that the fluid derived from processing amniotic tissue is a source of biologic proteins, growth factors and progenitor cells. Placental tissue is donated after cesarean birth and processed. The fluid obtained after the processing, has been shown to exhibit a variable cellular, growth factor and biologic protein content, which can significantly affect regenerative quality. Studies have observed there are no live progenitor cells present in preserved amniotic fluid allographs. The use of amniotic fluid allografts has been restricted in patients who were unable to use their own natural cells due to chronic illness, medication use, history of recent or active treatment of a malignancy, chemo or radiation therapy.
If you have been experiencing pain from a tendon that hasn’t improved, don’t wait until it’s too late. Dr. Luga Podesta can quickly determine the cause of your pain and provide the cutting edge regenerative orthopedic therapy necessary to get back in the game.
Ligament Injuries
What is the difference between a sprain and a strain?
 Sprains and strains are injuries that occur in soft tissue, however, the difference between sprains and strains lies within the tissue that they occur. Sprains occur in ligaments, whereas strains occur in muscles and tendons.
Sprains and strains are injuries that occur in soft tissue, however, the difference between sprains and strains lies within the tissue that they occur. Sprains occur in ligaments, whereas strains occur in muscles and tendons.
How are ligament injuries diagnosed?
Making a diagnosis of a ligament injury requires taking a detailed history describing the mechanism of injury location of pain and circumstances associate at the time of injury, hearing or feeling a pop for a tearing sensation in a particular joint. Performing a thorough dynamic joint stability exam with comparison to the non-injured side can be helpful when a ligament injury is suspected. Imaging studies such as stress x-rays, MRI scans or dynamic ultrasound valuations are important to detect any radiographic abnormalities as well as abnormalities specifically within a particular ligament with a suspected injury.
How are ligament injuries treated non-surgically?
The initial inflammatory phases are typically short lived and responsive to conservative treatment including the R.I.C.E. treatment principles plus: relative rest, oral NSAID medications, therapeutic physical modalities such as ice and heat, bracing to maintain stability and compression, elevation, protected movement and activity modification. However, for injuries that don’t respond to conservative treatments or with more severe cases when joint stabilization is priority, regenerative orthopedic injection procedures may be helpful to prevent the need for surgical stabilization procedures, prolonged recovery periods and delayed return to sports and normal function.:
- Platelet Rich Plasma (PRP) Treatments: Research has proven that Platelet rich plasma therapy can be a helpful treatment for mild and moderate ligament injuries. PRP, is performed to stimulate and further enhance our natural healing response when injected in an injury by concentrating growth factor containing platelets and circulating progenitor cells in plasma ultimately reducing pain and increasing tendon function by decreasing inflammation, stimulating ligament healing and functional improvement.
- Bone Marrow Concentrate (Progenitor cell) Treatment: Previously referred to as “Stem Cell Therapy”, progenitor cell-based treatments are reserved for more severe ligament conditions such as higher-grade acute sprains, chronic degenerative sprains or partial ligament tears. Collecting small amount of bone marrow from the patient. The marrow is concentrated and reinjecting back into the injury site or abnormal joint. Bone marrow concentrate in addition to PRP has shown promise to further diminish inflammation, promote and stimulate ligament growth not observed with PRP alone. Progenitor cell-based therapy is performed in regenerative orthopedics to enhance the body’s natural healing mechanisms and capabilities to treat orthopedic conditions involving tendons throughout the body.
- Amniotic Fluid Allographs: Amniotic tissue and amniotic membrane is a protective barrier in the human placenta. It is typically discarded after a baby is delivered. There is scientific evidence that the fluid derived from processing amniotic tissue is a source of biologic proteins, growth factors and progenitor cells. Placental tissue is donated after cesarean birth and processed. The fluid obtained after the processing, has been shown to exhibit a variable cellular, growth factor and biologic protein content, which can significantly affect regenerative quality. Studies have observed there are no live progenitor cells present in preserved amniotic fluid allographs. The use of amniotic fluid allografts has been restricted in patients who were unable to use their own natural cells due to chronic illness, medication use, history of recent or active treatment of a malignancy, chemo or radiation therapy.
If you have been experiencing pain from a ligament sprain that hasn’t improved, don’t wait until it’s too late. Dr. Luga Podesta can quickly determine the cause of your pain and provide the cutting edge regenerative orthopedic therapy necessary to get back in the game.
Arthritis
How is arthritis diagnosed?
Dr. Podesta can you confirm the diagnosis of arthritis after completing a thorough history and physical exam and imaging studies such as X-rays and possibly MRI. If a rheumatologic or infectious process suspected specific laboratory blood tests and joint fluid analysis maybe necessary to confirm diagnosis the specific cause.
What treatments are available for arthritis?
Treatment of arthritis is dependent on the stage of arthritis and the severity of symptoms. For mild arthritis with minimal symptoms, activity modification is often recommended and adequate to relieve mild symptoms. However, for more advanced cases with more severe symptoms, multiple nonsurgical and minimally invasive regenerative orthopedic treatments are available to maximize our bodies natural ability to repair and heal, ultimately relieving pain and improving function. Dr. Luga Podesta can determine the precise regenerative orthopedic therapy or combination of therapies that are best for you, including:
- Corticosteroid Injection: Cortisone injections have been used to relieve pain and treat inflammation conditions for years. These injections are most often performed in the physician’s office. These injections have been believed to be most effective in treating inflammatory arthritis, like rheumatoid arthritis. Cortisone is typically combined with local anesthetic medication such as lidocaine or Marcaine. Due to potential side effects and systemic risks such as articular cartilage damage, bone death (avascular necrosis), nerve damage, infection, elevation of blood sugar in diabetics, muscle tendon and ligament weakening; the number of injections you can receive in a year are limited.
- Viscosupplementation Injections: This is an injection or series of injections of a hyaluronan (hyaluronic acid) preparation into a joint for the treatment of arthritis. Hyaluronic acid is a natural substance in our joint fluid that assists in joint lubrication. It helps to provide a friction free surface allowing smooth movement of the articular cartilage covering the joint. Viscosupplementation injections can provide symptomatic pain relief while delaying the need for surgery.
- Platelet Rich Plasma (PRP) Treatments: Platelet rich plasma therapy is performed to stimulate and further enhance our natural healing response when injected in an injury by concentrating growth factor containing platelets and circulating progenitor cells in plasma ultimately providing a joint preservation affect by decreasing inflammation, reducing pain, stimulate healing and improve joint function.
- Progenitor cell (Bone Marrow Concentrate) Treatment: Previously referred to as “Stem Cell Therapy”, progenitor cell-based treatments begin by collecting small amount of bone marrow from the patient. The marrow is concentrated and reinjecting back into the injury site or abnormal joint. It is used to diminish inflammation, promote healing of articular cartilage and soft tissue such as meniscus, periarticular capsule, supporting ligaments and stimulate bone growth. It assists to reestablish a normal intraarticular environment, slow the degenerative process and help preserve the natural joint. Progenitor cell-based therapy is performed in regenerative orthopedics to enhance the body’s natural healing mechanisms and capabilities to treat a variety of orthopedic conditions involving joint and soft tissue.
- Interosseous Bioplasty Injection (IOBP): This is a regenerative orthopedic treatment that targets bone pathologies resulting from acute or chronic injury including osteoarthritis, persistent bone bruises, insufficiency fractions or avascular necrosis. The procedure is performed to stimulate physiologic subchondral bone remodeling, healing and involves delivering a combination of PRP, BMC and autologous thrombin into the injured bone. The treated bone is then protected over a 4-6 week period to optimize healing potential.
- Autologous Conditioned Serum: Autologous conditioned serum is performed by drawing a small sample of a patient’s own blood, allowed to remain in a clotted for at body temperature for 3 to 4 hours, centrifuged to separate the clot from its serum. The serum, which contains increased levels of autologous interleukin one receptor antagonist (IL1RA) is the injected back into the injured joint or tissue within 6 hours of the initial blood draw. IL1RA has been used in Europe since 2003 under the names Orthokine and Regenokine, is currently under investigation for the treatment of inflammatory conditions as a more natural and safer alternative to corticosteroids.
- Alpha 2 macroglobulin Injection (A2M): Alpha 2 macroglobulin is another regenerative orthopedic therapy being used more frequently to treat osteoarthritis. A2M provides joint preservation qualities when injected into a damaged joint higher at concentrations to target destructive enzymes. It is felt to help promote natural healing, tissue growth and prevent articular cartilage breakdown.
- Amniotic Fluid Allographs: Amniotic tissue and amniotic membrane is a protective barrier in the human placenta. It is typically discarded after a baby is delivered. There is scientific evidence that the fluid derived from processing amniotic tissue is a source of biologic proteins, growth factors and progenitor cells. Placental tissue is donated after cesarean birth and processed. The fluid obtained after the processing, has been shown to exhibit a variable cellular, growth factor and biologic protein content, which can significantly affect regenerative quality. Studies have observed there are no live progenitor cells present in preserved amniotic fluid allographs. The use of amniotic fluid allografts has been restricted in patients who were unable to use their own natural cells due to chronic illness, medication use, history of recent or active treatment of a malignancy, chemo or radiation therapy.
Neck & Low Back Pain
When does neck pain become concerning?
Most causes of neck pain will eventually resolve in a short period of time. However, if your pain is not improving, has been present for 4 or more weeks, is worsening or associated with any of the below symptoms, medical evaluation is recommended.
- Electric shock like pain radiating down your arm or behind the
- Inability to stand
- Worsening pain with movement of the neck
- Worsening numbness and or tingling in your arms or hands
- Night pain
When does low back pain become concerning?
Most causes of low back pain will eventually resolve in a short period of time. However, if your pain is not improving, has been present for 4 or more weeks, is worsening or associated with any of the below symptoms, medical evaluation is recommended.
- Electric shock like pain radiating straight down from your low back to your foot
- Inability to stand
- Worsening pain with sitting or lying down
- Worsening numbness and or tingling in your lower extremities
- Pain with walking
- Tearing or ripping sensation in abdomen or low back
When low back pain is associated with these “Red Flags”:
- Bilateral sciatic pain (electric shock like pain running down the back of your leg)
- Bowel or Bladder dysfunction (especially urinary retention)-may indicate Cauda Equina Syndrome
- Sexual dysfunction-may indicate Cauda Equina Syndrome
- Night pain awakening you from sleep associated with unexplained weight loss- may indicate a malignancy
- Failure of bed rest to relieve pain-may indicate underlying systemic disease
- Associated with a febrile illness- may indicate underlying systemic infection, focal disk space infection or osteomyelitis
If any of the above mentioned “Red Flags” are present, medical attention should be sought immediately!
What is the difference between diagnostic versus therapeutic spinal injections?
A precision diagnostic spinal injection can help diagnose the precise cause of neck and low back pain, resulting in pain relief that occurs immediately after the procedure is completed. However, the local anesthetic by itself is not expected to provide long-term pain relief. When the exact cause of the spinal pain has been determined by the diagnostic injection, a variety of therapeutic injections can then be performed at the precise location indicated by the diagnostic injection.
What types of therapeutic spinal injections are indicated for neck and low back pain?
When cervical or lumbar spinal pain is not resolving on its own or is not responding to conservative spinal interventions such as oral medication, the application of therapeutic modalities such as ice or heat or physical therapy, it may become to necessary consider therapeutic spinal injections. Once a precision diagnostic spinal injection has localized the cause of pain, specific therapeutic injection therapies can then be utilized to target the various areas of the spine to provide a longer lasting therapeutic effect. Examples of some of these image (ultrasound of fluoroscopy) guided spinal injections utilizing corticosteroid and anesthetic medications, radiofrequency nerve ablations, and regenerative orthopedic therapies such as platelet rich plasma or progenitor cell-based injections.
Some example of the therapeutic injections Dr. Podesta routinely performs include:
- Epidural and Caudal Injections: An epidural or caudal injection, places an anti- inflammatory steroid medication into the epidural space to decrease nerve root inflammation, to reduce pain in the low back and legs. By reducing inflammation, epidural injections help to promote healing an extended period of time.
- Cervical and Lumbar Facet Joint and Medial Branch/Dorsal Ramus Blocks: Not all spine pain emanates from the intravertebral disc or nerve roots. Facet joint pain is extremely common. Facet joint sensation including pain is transmitted from these joint to the brain by the median branch and dorsal ramus nerves. Blocking the transmission of pain signal from the facet joint to the brain with a short acting anesthetic, is extremely important diagnostic tool allowing us to precisely determine the exact location of the pain. Diagnostic median nerve and dorsal ramus blocks may be suggested when there is strong evidence to suspect the source of your pain is your facet joints.
- Radiofrequency Ablations: A radiofrequency ablation is a therapeutic procedure that uses an electrically generated radiofrequency current to generate heat that this disrupts the pain fibers of the median nerve and dorsal ramus that supplying sensation to the facet and sacroiliac joint. It is routinely performed to provide long-term relief for axial low back pain.
- Sacroiliac Joint Injections: The sacroiliac (SI) joints connect the lower spine (sacrum) with the pelvis (ilium). They transfer ground reaction forces from the lower leg and hip through the pelvis to the lumbar spine. Typically, these joints are very stable. However, the SI joints can move and undergo stress after restricted motion develops in the lumbar spine and hip. Image guided diagnostic SI joint injections with local anesthetic agents are used to determine if the joint is causing pain. The addition of a steroid medication or regenerative therapies such as PRP to diminish inflammation, a therapeutic effect can be provided.
- Lumbar Intervertebral Disc Injections: The intervertebral discs throughout the spine function to separate the vertebral bodies and exiting nerve roots. Disks can become painful when the lining of the disc known as the annulus tears and the nucleus, gel like structure within the disc leaks. Regenerative orthopedic procedures such as platelet rich plasma (PRP) and progenitor cell-based therapy with bone marrow concentrate (BMC) have proven beneficial in sealing, healing annulus tears and decreasing inflammation in and surrounding damaged discs.
These injections have been designed and are used clinically to diminish pain, improve function and prevent unnecessary spinal surgeries.
Can cell based therapies with PRP or progenitor cell-based treatments help?
Cell-based spinal therapeutic injections with platelet rich plasma (PRP) and progenitor cell (stem cell) therapies provide state of the art treatments for acute and degenerative spinal conditions which have the potential to stimulate the immune system and increase the body’s natural ability to heal damaged tissues such as intervertebral discs, diminish inflammation or facet joints, stabilize supporting spinal ligaments resulting in overall pain reduction and functional improvement. Cell-based therapies can provide patients with low back pain from a variety of causes with long-term relief from pain improving mobility and function with faster recovery times. Cell-based therapeutic spinal therapies can significantly reduce time away from family, sports, work or daily activities while delaying or completely avoiding the need for surgery and prescription medication.
Throwing Injuries
Experience matters! For the majority of his 30-year professional career, Dr. Luga Podesta has treated throwing athletes at the highest level. For 16 years he served as a team physician for the Los Angeles Dodgers and 3 years as a team physician for the Los Angeles Angels. Dr. Podesta is a renowned sports medicine physician specializing in the non-surgical treatment of orthopedic, musculoskeletal and sports-related injuries in throwing athletes involving the shoulder and elbow and has a wealth of experience returning throwers back to the field. Dr. Podesta continues to treat baseball players including Hall of Fame players, active major and minor leaguers, collegiate, high school and recreational players. Dr. Podesta has been a proponent for the non-surgical treatment of UCL injuries in throwers with cell-based therapies and published his research in the landmark paper “Treatment of Elbow Partial Ulnar Collateral Ligament Tears with Platelet Rich Plasma” in the American Journal of Sports Medicine, in 2013. Throwing related injuries can occur with one throw, or more commonly, as the result of multiple throws over a longer period of time, whether you are a professional athlete or a weekend warrior. How those injuries are treated and eventually heal will determine when and how well you can return to sports. Dr. Luga Podesta has both the experience and knowledge working and treating throwing athletes necessary to get you back in the game at the highest level of competition.
Common throwing injuries treated include:
- Shoulder pain
- Little Leaguer’s Shoulder (Humeral Growth Plate Fracture)
- Rotator Cuff Tendonitis
- Labral Tears
- SLAP Tears
- Shoulder Instability
- Elbow pain
- Little Leaguers Elbow (Medial Epicondyle Growth Plate Fracture)
- UCL sprains
- Tennis elbow (Tendonitis)
- Golfers Elbow (Tendonitis)
- Biceps Tendonitis
- Ulnar Nerve Instability
Dr. Luga Podesta is an expert in the diagnosis and treatment of the unique injuries that occur in overhand throwing athletes (baseball, softball, tennis, volleyball and water polo). He is an expert in the analysis and correction of throwing and hitting mechanics, which are necessary to return to play safely minimizing injury recurrence.
Sports Concussion
For over three decades, Dr. Luga Podesta has treated athletes at every age and level of competition with concussions and mild traumatic brain injury. Concussions can occur whether you are a competitive athlete, a weekend warrior or an adolescent. When and how quickly head injuries are recognized and treated, determine ultimate outcome and return to normal daily activity or sports. Choosing the correct doctor to evaluate and treat your concussion extremely important. Knowledge of the varying neurologic injuries, compromised neuropathic pathways and symptoms associated with even mild head injuries and concussion are invaluable when decisions must be made regarding treatment, activity modification and eventual safe return back to the normal life. Dr. Podesta will utilize cutting age diagnostic tools combined with evidence based medical treatments to optimize your recovery.
Concussion “RED FLAGS”
Severe head injuries can result in several “Red Flags” that require immediate emergency department evaluation and possible advanced brain imaging such as MRI of CT scans. The presence of any of the below signs or symptoms require immediate medical evaluation.
- Loss of consciousness
- Altered mental status
- Suspected spine injury
- High-speed injury (motor vehicle accident, fall from height)
- Worsening headache despite resting
- Weakness in any extremity
- Visible bump on head boney defect of school
How are concussions initially treated?
When a concussion is suspected, the athlete should be immediately removed from the remainder of the athletic competition or activity. A thorough neurocognitive evaluation should be performed immediately, and the brain should be allowed to rest until symptoms subside. Return to sports or activity is restricted until the brain has been allowed to rest and the athlete is completely symptom-free at rest and after completing a post-concussion “Return to Play” protocol.
Recovery guidelines after sustaining a concussion.
- The Immediate removal from sports, physical activity Will high-risk activities when a head injury occurs when a concussion is suspected.
- Initial imaging studies such as MRI or CT scans are not necessary unless there is a loss of consciousness or severe neurological symptoms.
- Get adequate sleep! There is no need to wake up during the night.
- Limit exposure to TV, telephone computers and video games. This is important to allow the brain to rest.
- To Evaluate for modification of school for work to prevent worsening of symptoms.
- Light aerobic activity such as walking. Recent studies have shown that light aerobic activity can help children recover faster from a concussion.
When is an athlete cleared to return to sports?
Once the athlete is asymptomatic and back to normal activities including school, and cleared to return sports by their physician, the return to sports process can begin. The concussed athlete is placed into a progressive, stepwise, supervised, “Return to Play” post-concussion protocol over a 5-day period. If the athlete is able to progress through the activity-based program symptom free, they are typically considered cleared to safely return to competition.
Diagnostic Ultrasound Imaging
Determining an accurate diagnosis is imperative before an injury specific treatment can be implemented. Dr. Podesta will utilize the most advanced point of care diagnostic and therapeutic image guided treatments available to optimize overall outcomes. Musculoskeletal ultrasound is a devise that assists us visualizing most anatomic structures or injuries immediately without the risk of ionizing radiation.
What are the advantages of Ultrasound?
- Ultrasonic images make it possible to more accurately diagnose and treat a wide scope of injuries and conditions.
- Produce high-resolution soft tissue images with better resolution than MRI imaging in real time.
- Facilitate dynamic examination of anatomic structures.
- Allows for interaction with the patient during the examination.
- Images are minimally affected by metal artifact.
- Enables for rapid side to side comparison.
- Equipment is portable.
- No radiation, is safe, no know contraindications for use.
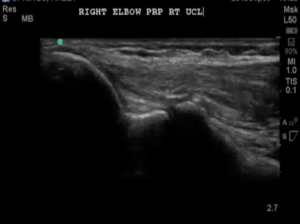
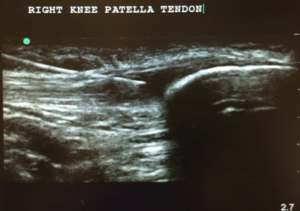
Ultrasound Guided Injections
Ultrasound-guided procedures have become the standard of care permitting safe and precise needle placement when treating a wide range of conditions affecting ligaments, muscles, tendons and joints. Several studies have shown that ultrasound guidance assure accuracy while performing regenerative orthopedic injections, corticosteroid or viscosupplementation injections in joints or soft tissue such as tendons and ligaments.
Fluoroscopic Guided Injections
Fluoroscopic guidance has been used for many years to accurately and safely guide needles for a variety of procedures where precise needle placement is absolutely necessary such as diagnostic or therapeutic spinal procedures. Fluoroscopic guidance is also widely utilized during orthopedic procedure when ultrasound needle guidance is inadequate, such as injecting into a bone.
What is the difference between diagnostic versus therapeutic spinal injections?
A precision diagnostic spinal injection can help diagnose the precise cause of neck and low back pain, resulting in pain relief that occurs immediately after the procedure is completed. However, the local anesthetic by itself is not expected to provide long-term pain relief. When the exact cause of the spinal pain has been determined by the diagnostic injection, a variety of therapeutic injections can then be performed at the precise location indicated by the diagnostic injection.
What types of therapeutic spinal injections are indicated for neck and low back pain?
When cervical or lumbar spinal pain is not resolving on its own or is not responding to conservative spinal interventions such as oral medication, the application of therapeutic modalities such as ice or heat or physical therapy, it may become to necessary consider therapeutic spinal injections. Once a precision diagnostic spinal injection has localized the cause of pain, specific therapeutic injection therapies can then be utilized to target the various areas of the spine to provide a longer lasting therapeutic effect. Examples of some of these image (ultrasound of fluoroscopy) guided spinal injections utilizing corticosteroid and anesthetic medications, radiofrequency nerve ablations, and regenerative orthopedic therapies such as platelet rich plasma or progenitor cell-based injections.
Some examples of the therapeutic injections that Dr. Podesta routinely performs include:
- Epidural and Caudal Injections: An epidural or caudal injection, places an anti- inflammatory steroid medication into the epidural space to decrease nerve root inflammation, to reduce pain in the low back and legs. By reducing inflammation, epidural injections help to promote healing an extended period of time.
- Cervical and Lumbar Facet Joint and Medial Branch/Dorsal Ramus Blocks: Not all spine pain emanates from the intravertebral disc or nerve roots. Facet joint pain is extremely common. Facet joint sensation including pain is transmitted from these joint to the brain by the median branch and dorsal ramus nerves. Blocking the transmission of pain signal from the facet joint to the brain with a short acting anesthetic, is extremely important diagnostic tool allowing us to precisely determine the exact location of the pain. Diagnostic median nerve and dorsal ramus blocks may be suggested when there is strong evidence to suspect the source of your pain is your facet joints.
- Radiofrequency Ablations: A radiofrequency ablation is a therapeutic procedure that uses an electrically generated radiofrequency current to generate heat that this disrupts the pain fibers of the median nerve and dorsal ramus that supplying sensation to the facet and sacroiliac joint. It is routinely performed to provide long-term relief for axial low back pain.
- Sacroiliac Joint Injections: The sacroiliac (SI) joints connect the lower spine (sacrum) with the pelvis (ilium). They transfer ground reaction forces from the lower leg and hip through the pelvis to the lumbar spine. Typically, these joints are very stable. However, the SI joints can move and undergo stress after restricted motion develops in the lumbar spine and hip. Image guided diagnostic SI joint injections with local anesthetic agents are used to determine if the joint is causing pain. The addition of a steroid medication or regenerative therapies such as PRP to diminish inflammation, a therapeutic effect can be provided.
- Lumbar Intervertebral Disc Injections: The intervertebral discs throughout the spine function to separate the vertebral bodies and exiting nerve roots. Disks can become painful when the lining of the disc known as the annulus tears and the nucleus, gel like structure within the disc leaks. Regenerative orthopedic procedures such as platelet rich plasma (PRP) and progenitor cell-based therapy with bone marrow concentrate (BMC) have proven beneficial in sealing, healing annulus tears and decreasing inflammation in and surrounding damaged discs.
These injections have been designed and are used clinically to diminish pain, improve function and prevent unnecessary spinal surgeries.
Can cell based therapies with PRP or progenitor cell-based treatments help?
Cell-based spinal therapeutic injections with platelet rich plasma (PRP) and progenitor cell (stem cell) therapies provide state of the art treatments for acute and degenerative spinal conditions which have the potential to stimulate the immune system and increase the body’s natural ability to heal damaged tissues such as intervertebral discs, diminish inflammation or facet joints, stabilize supporting spinal ligaments resulting in overall pain reduction and functional improvement. Cell-based therapies can provide patients with low back pain from a variety of causes with long-term relief from pain improving mobility and function with faster recovery times. Cell-based therapeutic spinal therapies can significantly reduce time away from family, sports, work or daily activities while delaying or completely avoiding the need for surgery and prescription medication.
Experience matters! Injuries can occur whether you are a competitive athlete, weekend warrior, musician, dancer or homemaker. Choosing the correct physician to evaluate, diagnose and treat your injury is paramount to safely return you back to the activities you enjoy. I have both the experience and knowledge necessary to get you back to what you love, utilizing personalized, cutting edge non-surgical treatments designed to stimulate and enhance your body’s natural healing capabilities …. Luga Podesta, MD
Frequently Asked Questions (FAQs)
Tendon Injuries
Tendonitis:
Tendinitis is an acute inflammatory condition affecting tendons typically where they attach on a bone. It is described by several names including tennis elbow, golfers’ elbow, jumpers’ knee or swimmers’ shoulder. Regardless of the name, tendinitis can be painful, debilitating and effect any tendon. Early treatment is extremely important to minimize the long-term risks and effects of tendon injury. Dr. Luga Podesta has both the experience, knowledge, and skill to minimize those risks. Dr. Podesta is a regenerative orthopedic and sports medicine expert with over 3 decades of experience who can offer cutting edge regenerative medicine and orthopedic treatments to stimulate and enhance tendon healing to improve your body’s natural healing capacity.
What is Tendinosis?
Tendinosis develops when the inflammatory process for several weeks or months, is in adequately treated and allowed to progress. The thick resilient, cord like tendon tissue undergoes degenerative structural changes and new abnormal blood vessel growth, leading to loss of tensile strength to withstand the stresses placed upon it. Without proper treatment, the tendon is predisposed to further injury including rupture. Typically, pain is described as dull and achy, worsening with movement of the affected joint and is tender to touch.
What is calcific tendonitis?
Calcific tendinitis is an extremely painful and debilitating disorder characterized by the development and deposition of hydroxyapatite (a crystalline calcium phosphate) in any tendon of the body. Although this could develop in any tendon in the body, it most commonly develops in the tendons of the shoulder rotator cuff tendons. It occurs in 30 to 40-year old’s, and in patients with diabetes.
Ligament Injuries
Ligament Injuries:
Ligaments are bands of connective tissue bundles consisting of collagen and elastic fibers surrounded by dense protective sheaths. Ligaments function to provide stability and support to the many joints of the body. They connect joints together, while maintaining joint stability from the tremendous applied forces occurring with normal daily activity and sports. When an injury to a ligament occurs, commonly referred to as a sprain, joint stability becomes compromised. Without early recognition and treatment, chronic instability can lead to articular cartilage and eventually joint destruction. Early treatment is extremely important to minimize the long-term risks and effects of ligament injury.
What is a sprained ligament?
A ligament sprain occurs when the ligament ligament fibers are over stretched or in more severe cases, tearing of the ligament occurs. Ligaments are viscoelastic structures, meaning they can gradually stretch or lengthen when under tension, but then return back to their original shape and length when that tension is removed. When the stretch is too great or occurs for too long a period of time, the ligaments cannot retain its original shape destabilizing the joint. Sprains are classified as a grade 1, mild; Grade 2, moderate and grade 3, severe or complete disruption of the ligament. Sprains can occur in any joint of the body. The most common parts of the body affected by sprains include the ankle, knee, elbow, shoulder, hand and wrist.
What common activities lead to sprains?
Sprains occur in many different joints, and typically result from an acute over stretching of a ligament or abnormal stress from a direct blow, pivot or twisting activity. Sprains can also result from the gradual stretching, resulting from prolonged repetitive applied tension delivered to a ligament commonly resulting from repetitive overuse activities. Sprains frequently occur under these common circumstances including:
- Ankle: Landing awkwardly on a jump; Walking or running on uneven surfaces
Knee: Pivoting during an athletic event: Direct blow to the outside or inside of the knee with the foot planted. - Elbow: Throwing a ball repetitively; Tackling with an outstretched arm.
- Shoulder: Diving and landing on an outstretched arm; Throwing a ball
Thumb: Twisting while gripping a ski pole or racquet.
Can children sprain a ligament?
“Kids don’t sprain they break”! Skeletally immature children will often fracture through a “growth plate”, which are growth centers near the end of bones, before they sprain a ligament. Growth plate fractures are often mistaken for sprained ligaments in children and are some of the most commonly missed fractures in emergency departments. Although the mechanism of injury is the same to cause a sprain in an adult, Growth plates in children typically are weaker than the associated ligaments that support them, and fracture before the ligament injury can occur. It’s easy to remember, “kids don’t sprain they break”!
Arthritis
Arthritis:
Osteoarthritis is the most common form of arthritis and affects millions of individuals worldwide. Arthritis is a chronic progressive disease that effect the articular cartilage of joints.. It is associated with abnormal wearing, degeneration and permanent loss of the protective articular cartilage cushion in a joint and a chemical imbalance of inflammatory and anti-inflammatory proteins within the knee. It develops slowly and progresses over time, resulting in joint pain, stiffness, loss of joint flexibility and swelling.
What is arthritis?
Any joint in our body can develop arthritis. Arthritis can develop in any joint, however it most commonly affects joints in the knees, hip, shoulder, spine and hands. Arthritis can occur due to traumatic injuries, or as a result of a surgical procedure such as an ACL or injury surgery. Arthritis can also develop as a result of rheumatologic or inflammatory diseases such as rheumatoid arthritis. Osteoarthritis is the most common form of arthritis. Other common forms of arthritis include post traumatic arthritis, rheumatoid arthritis and psoriatic arthritis. A biochemical imbalance occurs within the joint itself or supporting soft tissues leading to inflammation and progressive permanent joint disruption.
What are the symptoms of arthritis?
Symptoms due to arthritis can’t appear at any time but most often develop slowly and worsened over time. Symptoms can also change or worsen as a result of weight gain, after a traumatic event or illness. Common symptoms include:
- Pain or soreness – occurring or worsening with or after activity, or at night
- Development of a grating or clicking sensation with movement
- Swelling – can range from mild to significant increasing pain and restricting ability to bend
- Stiffness
- Loss of joint range of motion
- Joint instability,
- Malalignment and deformity
Neck & Low Back Pain
Neck and Low Back Pain
Neck pain affects millions of people each year around the world. In most cases, neck pain does not arise from a serious condition, is self-limiting and subsides in several days. The neck or cervical spine is made up of several boney vertebrae separated by cervical intervertebral discs that support the head, ligaments and muscles that stabilize the joints, absorb pressure and allow for motion. The cervical vertebrae encase and protect the spinal cord, and spinal nerves, and is further supported be overlying ligaments and muscle. Anyone of these structures is vulnerable to injury and can result in neck pain or stiffness.
What causes neck pain?
Neck pain and stiffness can result from the supporting muscles and ligaments, intervertebral discs, nerves, boney structures, joints, ligaments or may be referred from other areas of the body such as the shoulder, lungs or heart. Most commonly neck pain results from repetitive, prolonged or strenuous exercise such as lifting, standing, bending, twisting, carrying heavy objects, or direct blows to the top of the or quick and forceful, sudden movements of the neck. Pain and stiffness can result from overuse, repetitive use, acute or chronic injury, compression of a structure such as nerves around the neck (pinched nerve) or an inflammatory process. Most neck pain is acute, short-lived and lasts only a few days or a few weeks. It is extremely important that the exact structure or structures causing pain are determined and specifically treated. Often the standard clinical history, physical examination and imaging studies such as x-rays, CT scans and MRIs are not entirely sufficient to determine where the pain is actually coming from. Often, diagnostic cervical spinal injections are necessary to pinpoint the exact location of the pain generator allowing for precise targeted treatment.
Common structures that can cause low back pain include:
- Cervical supporting musculature
- Intervertebral discs (herniations/bulges)
- Cervical facet joint arthritis (spondylosis) and supporting ligaments
- Cervical spinal fractures
- Degenerative cervical disc disease
- Nerve root compression / Radiculopathy (Pinched nerves)
- Spinal stenosis
- Vertebral artery syndrome
- Tumors
Low Back Pain
Back pain is second only to the common cold as the most common reason for seeing a physician. Low back pain is a very common problem experienced by most individuals. 80% of the world’s population will experience low back pain sometime during their lives and there are many causes of low back pain. Most low back pain is acute, short-lived and lasts only a few days or a few weeks. When back pain doesn’t get better, is severe or remains chronic and restricts you from activities that you enjoy, it’s time to seek out professional care. Dr. Luga Podesta has both the experience and knowledge necessary to get you back to the activities you enjoy. Dr. Podesta is a regenerative orthopedic expert with over 3 decades of experience treating back pain non-surgically and can provide a comprehensive functional and biomechanical evaluation to determine the cause of your pain, followed by a holistic treatment and rehabilitation program including cutting-edge regenerative orthopedic treatments to stimulate and enhance your body’s natural healing capacity without surgery.
What causes low back pain?
There are many causes of low back pain. Most low back pain is acute, short-lived and lasts only a few days or a few weeks. There are a number of structures or combination of structures in the lumbar spine that can generate pain including the supporting muscles and ligaments, intervertebral discs, nerves, boney structures, joints, ligaments and infection. Pain can also be referred from other areas of the body. The most common causes of low back pain can result from repetitive, prolonged or strenuous exercise such as lifting, standing, bending, twisting, carrying heavy objects, or sitting for long periods of time.
It is extremely important that the exact structure or structures causing pain are determined and specifically treated. Often the standard clinical history, physical examination and imaging studies such as x-rays, CT scans and MRIs are not entirely sufficient to determine where the pain is actually coming from. Often, diagnostic lumbar spinal injections are necessary to pinpoint the exact location of the pain generator allowing for precise targeted treatment.
Common structures that can cause low back pain include:
- Lumbar supporting musculature
- Intervertebral discs
- Lumbar vertebrae
- Lumbar facet joints and supporting ligaments
- Lumbar spinal fractures
- Lumbar spondylolisthesis
- Degenerative lumbar disc disease
- Nerve root compression
- Spinal stenosis
- Sacroiliac joint
- Abdominal aortic aneurism
- Tumors
Sports Concussion
What is a concussion?
A concussion is defined as a traumatically induced transient loss of brain function. Concussions are further defined as a subclass of traumatic brain injuries or TBI. Sudden forceful movement can result in the brain striking or twisting within the skull, creating chemical imbalances and damage to brain cells. The Centers for Disease Control CDC estimates approximately 3.8 million concussions occur yearly in the United States as a result of participation in competitive and recreational sporting activities.
How does a concussion occur?
The two most common mechanisms of injury leading to concussions are either a direct blow to the head, or an indirect rotational force of the body and head. Forces resulting in either a direct blow to the head leading to brain-skull contact or an indirect force due to a rotational or twisting injury to the head and torso causing sheering force within the brain result in cellular damage and disruption. Either mechanism of injury can produce concussive symptoms.
Who is at risk for a concussion?
Anyone may experience a blow to the body or head or a fall significant enough to cause a concussion. However, individuals are at greater risk for these injuries if they participate in collision sports like football, ice hockey, lacrosse, Soccer or rugby. Women are at a greater risk then men for sustaining a concussion. Playing fatigued or injured or having sustained a prior concussion also increases the risk of future concussion.
What are the signs and symptoms of concussion?
Signs and symptoms of concussion can vary between individuals and can appear immediately after the injury or take 2 to 3 days to develop. Symptoms of concussion include but are not limited to:
- Headaches or pressure feeling in the head
- Confusion or “foggy” feeling
- Blurred vision
- Dizziness
- Nausea
- Vomiting
- Delayed response to questions/feeling slowed
- Fatigue
- Concentration and memory loss
- Irritability and personality changes
- Sensitivity to light and sound
- Difficulty sleeping
- Psychological adjustment problems, mood irritability and depression
- Disorders of taste and smell

